What is a Facet Joint Injection?
how we can help
Facet Joint Injection Overview
Facet Joint Injection A facet joint injection is a medical procedure in which a local anesthetic and a steroid medication are injected into one or more of the small joints located between the vertebrae of the spine, called the facet joints. The goal of the injection is to alleviate pain and inflammation in the facet joint and surrounding tissues.
Facet joint injections are also referred to as intraarticular facet joint injections, zygapophysial joint injections, or facet injections. They are typically administered under fluoroscopy, a type of X-ray imaging, or ultrasound guidance to ensure accurate placement of the medication. A facet joint injection is usually performed on an outpatient basis and takes only a few minutes to complete.
The facet joints are located along the entire length of the spine. Facet joint sets extend from the rear of the vertebrae in pairs. The facet joint interlocks with adjacent vertebrae on the upper left and right and the lower left and right.
The primary function of the facet joints is to provide mobility, stability, and balance to the spine. The facet joints provide the spine with a range of motion but are rigid enough to protect the spinal cord and the exiting nerve roots.
There are many conditions that may lead to pain and inflammation in the facet joints. Facet joint osteoarthritis (OA) is the most frequent cause of facet joint pain. Facet joint degeneration happens when the cartilage between the two joints deteriorates, and bone begins to rub against bone. Serious pain can occur in the neck, upper back, or lower back.
Depending on where the arthritis is found, it may be harder for the patient to move their neck, back, or hips. This makes walking, sitting, or looking around much more difficult. Facet joint arthritis can significantly impact the efficacy of injection therapies aimed at alleviating pain and improving mobility.
Another condition that impacts the facet joints is Spondylolisthesis. This condition occurs when a spinal vertebra slips forwards or backwards in relation to the adjacent vertebra. Abnormal spinal alignment puts stress on the facet joints, leading to pain and discomfort. Other conditions that may cause facet joint pain are spinal stenosis, or trauma and injury, such as whiplash.
Possible candidates for facet joint injections include patients who have experienced moderate to severe facet pain lasting three months or longer and have not responded to non-surgical treatments, such as pain-relieving medication and physical therapy.
Table of Contents
Treats
Diagnosing
Recovery
Patients Ask:
How are facet joint injections used to treat back pain?
Texas Back Institute Responds: Initially, a facet joint injection may be administered for diagnostic purposes. To properly diagnose facet joint pain, a diagnostic facet joint injection may be used. If the pain significantly decreases after receiving the injection, it confirms that the facet joint is the cause of the pain. Beyond their diagnostic value, facet joint injections are a therapeutic intervention that can provide temporary pain relief. By targeting pain, a patient is better able to participate in physical therapy and other rehabilitative and conservative care treatments.
Lumbar Facet Joint Disorders
The lumbar spine (low back) is the spinal region most susceptible to facet joint syndrome. This is due to the lower back’s role in supporting the weight of the upper body and transferring it to the lower extremities. In addition, the lumbar muscles and vertebrae provide flexibility that allows the trunk to move in various directions – forward, backward, side-to-side, and rotation. As a result, the facet joints in this spinal region are subject to a high degree of age-related “wear and tear,” causing irritation and inflammation that lead to pain and discomfort. Facet joint injections are commonly used to manage chronic spinal pain by alleviating pain and improving patient mobility over extended periods.
Many painful conditions can affect the lumbar facet joints, including facet arthropathy, an arthritic condition that can cause lower back pain. Lumbar facet joint disorders cause pain that is characterized as a localized ache with some degree of stiffness. Patients report that pain is usually worse in the morning (link to blog post on morning back pain) or after periods of inactivity. Radicular leg pain, or sciatica, may occur from spinal nerve root impingement. Other symptoms include tenderness on palpitation and worsening of pain in certain postures or specific activities.
Many symptoms of facet joint disorders are like other lower back conditions, including degenerative disc disease. These conditions can occur simultaneously, causing overlapping symptoms, and adding a degree of complexity to the diagnostic process.
Patients Ask:
How are lumbar facet joint disorders diagnosed?
Texas Back Institute Responds: Diagnostic imaging tests like X-rays, CT scans, and MRIs can disclose facet joint changes that are consistent with osteoarthritis. A facet joint injection can provide physicians with diagnostic information. If the pain subsides after receiving the injection, it confirms that the facet joint is, indeed, the source of the pain.
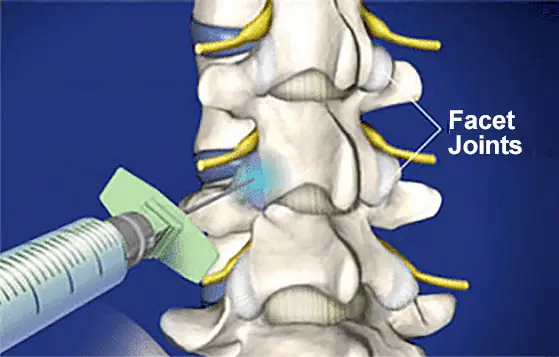
(insert illustration of syringe inserted in the facet joint)
Lumbar Facet Joint Injections
A lumbar facet joint injection, also known as a lumbar facet joint block, is a standard procedure. A local anesthetic agent, or numbing medicine, is injected into the facet joints. This can offer immediate pain relief due to the anesthetic used during the procedure. Depending on the severity of the condition and how many joints are involved, several injections may be needed.
Lumbar facet injections are typically given to patients who are experiencing arthritic pain in their facet joints. However, patients with mechanical lower back pain may also benefit from these injections.
Cervical Facet Joint Injections
Cervical facet syndrome is a condition caused by inflammation or damage to the facet joints in the neck. This can lead to pain, stiffness, and even headaches (link to blog page on misdiagnosis of migraines). As the cervical spine degen`erates with age, other changes also take place in the neck.
The cervical spine may begin to experience excessive motion due to disc and joint degeneration. This can cause irritation of the facet joints in the cervical spine and result in pain and inflammation.
Cervical facet joint disorders are diagnosed by reviewing a patient’s medical history, a thorough physical examination, and diagnostic imaging tests like an X-ray, CT scan, or an MRI.
Cervical facet injections are a standard medical procedure performed on an outpatient basis. The duration of pain relief after a cervical facet joint injection can vary from person to person, however, many individuals experience pain relief for several weeks to several months.
(insert photo or illustration of the neck area of the spine)
Patients Ask:
What if facet joint injections don’t stop the pain? What then?
Texas Back Institute Responds: Facet joint injections are a safe and effective way to treat chronic back or neck pain without surgery. However, some patients do not achieve relief with these injections. If this is the case, the first step will be to do further diagnostic testing. Epidural steroid injections can also help reduce inflammation and pressure on a nerve or nerves resulting from a herniated disc, spinal stenosis, or other spinal issues. Radiofrequency ablation is another treatment option for treating back pain when facet injections don’t work. This treatment is used to prevent spinal nerves from sending pain signals to the brain.

The Procedure for Facet Joint Injections
During the injection procedure, the patient will be lying on their stomach on a padded table in the procedure room. If IV sedation is used, monitoring equipment such as EKG pads and a blood pressure cuff will be placed, along with nasal oxygen tubing. The area of injection will be washed with a cool room temperature liquid antiseptic cleaning solution. A local anesthetic will be used to numb the area of the injection.
Fluoroscopy, a method used to make images with x-rays, will be used by the physician to accurately place the needle at the facet joint(s) being injected. A mixture of anesthetic and cortisone is injected into the facet joint(s). The injection procedure will typically take about 15-30 minutes. After the procedure, the patient will be transported back to the recovery area.
Patients Ask:
What should I expect when I get home after the procedure?
Texas Back Institute Responds: During the immediate hours after the procedure, the area of the spine where the injection was placed can feel a little weak or odd because of the numbing effect of the injection.
Additionally, some soreness from the needle injection site is expected and can last a few days. Icing the area for 20 minutes at a time, as needed, for the first couple of days afterward is recommended. After a few days, ice or heat can be used based on patient preference.
When Is Surgical Intervention Suggested
At Texas Back Institute, surgery is always the last treatment option suggested. Surgery for signs and symptoms caused by facet joint problems is rare, but may be advised in the following situations:
- Presence of conditions that naturally accompany other conditions, such as symptomatic lumbar spinal stenosis (narrowing of the bony openings for spinal nerves), lumbar degenerative disc disease, or lumbar herniated discs.
- Severely fractured or displaced facets that cannot be managed by nonsurgical methods.
- Spinal tumors or cysts.
- Cauda equina syndrome, which is compression of the spinal nerves that descend from the spinal cord.
Surgery for lumbar facet joint syndrome may require a laminectomy. Laminectomy surgery is the removal of the posterior part of the vertebra and may be used in facet disorders that lead to spondylolisthesis. A laminectomy surgery restores the space for neural tissues and relieves nerve compression. When treating conditions such as spondylolisthesis, a minimally invasive fusion surgery using lumbar instrumentation, or spinal implants may be necessary to stabilize the motion segment.
Recovery From Facet Joint Injection
Texas Back Institute is recognized as a world leader in getting people back to life, most without ever requiring surgery. In fact, nine out of ten of our patients recover with non-surgical back pain treatment.
A facet joint injection is a minimally invasive procedure that has the potential to reduce back or neck pain for months. After a facet joint injection, physical therapy is recommended to continue to rehabilitate the spine.
Patients Ask:
What kind of physical therapy will I need?
Texas Back Institute Responds: Most patients begin a program that includes gentle mobility exercises, core strengthening, and spinal stabilization exercises. Individualized recommendations are made based on your specific condition and overall health.
Why Wait?
If back pain is interfering with your quality of life, it might be time to talk to an expert at Texas Back Institute and set an appointment.
Learn more
Frequently Asked Questions
Initially, a facet joint injection may be administered for diagnostic purposes. To properly diagnose facet joint pain, a diagnostic facet joint injection may be used. If the pain significantly decreases after receiving the injection, it confirms that the facet joint is the cause of the pain. Beyond their diagnostic value, facet joint injections are a therapeutic intervention that can provide temporary pain relief. By targeting pain, a patient is better able to participate in physical therapy and other rehabilitative and conservative care treatments.
Diagnostic imaging tests like X-rays, CT scans, and MRIs can disclose facet joint changes that are consistent with osteoarthritis. A facet joint injection can provide physicians with diagnostic information. If the pain subsides after receiving the injection, it confirms that the facet joint is, indeed, the source of the pain.
Facet joint injections are a safe and effective way to treat chronic back or neck pain without surgery. However, some patients do not achieve relief with these injections. If this is the case, the first step will be to do further diagnostic testing. Epidural steroid injections can also help reduce inflammation and pressure on a nerve or nerves resulting from a herniated disc, spinal stenosis, or other spinal issues. Radiofrequency ablation is another treatment option for treating back pain when facet injections don’t work. This treatment is used to prevent spinal nerves from sending pain signals to the brain.
During the immediate hours after the procedure, the area of the spine where the injection was placed can feel a little weak or odd because of the numbing effect of the injection.
Additionally, some soreness from the needle injection site is expected and can last a few days. Icing the area for 20 minutes at a time, as needed, for the first couple of days afterward is recommended. After a few days, ice or heat can be used based on patient preference.
Most patients begin a program that includes gentle mobility exercises, core strengthening, and spinal stabilization exercises. Individualized recommendations are made based on your specific condition and overall health.
Locations