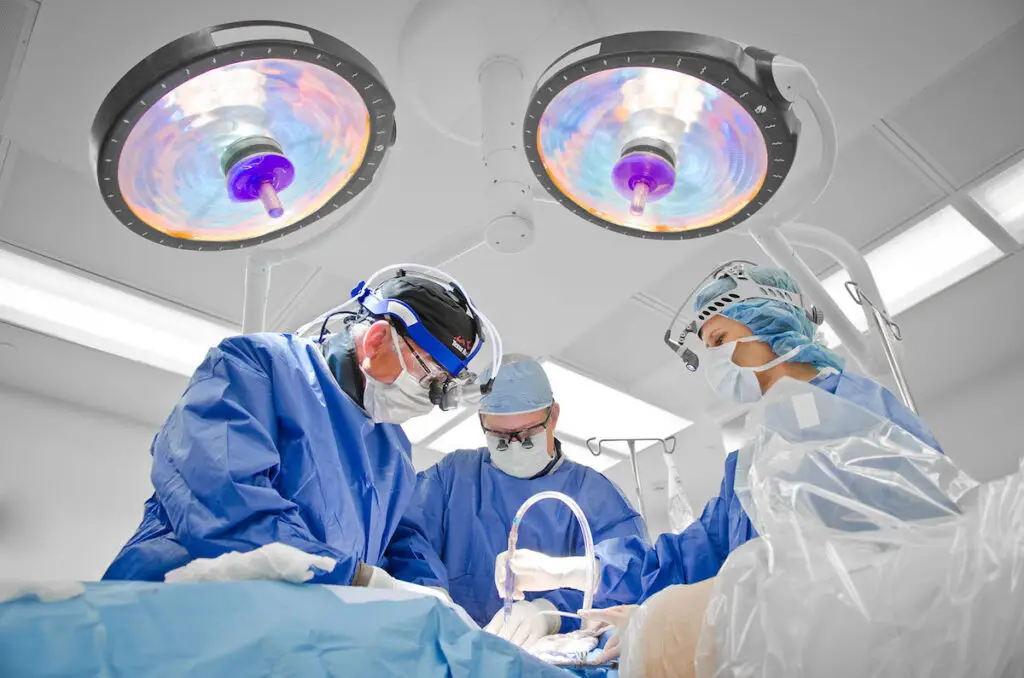
One of the most remarkable advancements in medical technology and spinal treatment occurred more than 20 years ago. At the request of the Federal Drug Agency (FDA), leading spine surgeons at selected practices around the United States began exploring the feasibility of replacing damaged vertebral discs with those that were man-made.
An artificial disc is an elegant concept because it restores motion between the vertebral bodies instead of fusing them to other discs and locking them in place. However, improving on what Mother Nature “created” is always a challenge. Fortunately, the spine specialists at Texas Back Institute (TBI) were up for the task.
While surgery is the final option considered by the spine experts at Texas Back Institute, state-of-the-art treatment can help relieve pain and change lives. If you have neck or back pain, click here to see an expert.
Three Experts Discuss Disc Replacement
Recently, three Texas Back Institute colleagues—Dr. Richard Guyer, Dr. Scott Blumenthal, and Dr. Jessica Shellock—sat down to discuss the history and impact of the artificial disc replacement procedure.
Dr. Guyer, one of the founders of Texas Back Institute and a participant in the early FDA trials, acted as the discussion leader, while Drs. Blumenthal and Shellock added context and surgical insights. “How did the artificial disc replacement procedure come about?” Dr. Guyer asked.
“We started looking at it, at least experimentally, back in the 1990s,” Blumenthal said. “In March of 2000, we started doing disc replacements at TBI. For more than 23 years, we’ve done more and learned more each time we perform the procedure.
Dr. Shellock explained what artificial disc replacement entails.
“A disc replacement involves the surgical removal of a native disc, and in the space where the disc once was, we insert a device that allows the spine to maintain movement,” she said.
“Most everyone has heard of spinal fusion, and many understand that motion is taken away from the spinal segment when this is performed. The disc replacement, also known as disc arthroplasty, involves implanting a man-made disc made of metal, ceramic or plastic. That device allows for motion to continue, enabling the movement of the spine.”
“We perform this procedure in the neck, or cervical spine, and in the lower back, or lumbar area,” Blumenthal added. “Interestingly, this ‘replacement’ concept is not new. In the ‘old days,’ orthopedic surgeons would fuse hip and knee joints as a treatment for arthritis. Now, these replacement joints have become standard practice. The disc replacement has become a natural evolution. The joints were meant to move.”
We did the first disc replacement 23 years ago, “Guyer noted. “Any idea of how many procedures we have done so far?”
“Based on the most recent numbers, over 5,000 patients have been implanted with artificial discs,” Shellock said. “That includes more than 6,000 implants for those patients. This means we have vast experience at Texas Back Institute in doing disc replacement.”

The Learning Curve
“For those of us who have been performing this disc replacement procedure for more than 20 years, it seems counterintuitive to realize that many fusion procedures are still being performed,” Guyer said. “Why do you think there are still so many fusions being done?”
“There is a learning curve,” Blumenthal said. “And some surgeons are less willing to get out of their comfort zone. Those of us who have been doing spine surgery for many years were originally trained in the fusion procedure. There is also an economic consideration. Fusion surgery is more lucrative than disc replacements.”
More Cervical Procedures
“I’ve noticed another interesting trend,” Guyer said. “There seems to be many more cervical procedures as compared to lumbar procedures. Why is that?”
“One word,” Blumenthal said, “Diagnosis. The symptoms that suggest cervical disc replacement have been dealt with by almost every surgeon. Classically, we treated this with non-motion options (such as fusion), but now we have motion options. Lumbar spine is a different issue. It basically involves an arthritic, painful joint that causes back pain without neurologic issues. Some surgeons elect to not treat this.”
Shellock added, “It is also a familiar approach to get to the cervical spine, and most surgeons feel comfortable with that. Whereas, with the lumbar spine, we partner with ‘access surgeons,’ whose job is to gain access to the area. Not all surgeons have that capability or have access to these specialists. Because of the talent we have in-house at TBI, we have certainly benefited from having access to these specialists.”
“We also see patients regularly who say that their surgeon never offered the option for disc replacement in the lumbar area,” Guyer noted. “Why is that?”
“Two reasons,” Blumenthal offered. “First, in the lumbar or lower back area, TBI has become a center of excellence for disc replacement. People come from all over the country to TBI. Secondly, with cervical spine procedures, there is much less reimbursement for disc replacement than there is for fusion. Again, there is an economic consideration.”
Shellock added, “The technical aspect of doing this type of procedure well is something that requires a lot of repetition—many procedures—to have adequate experience, especially with the lumbar spine. A disc replacement in the lumbar area is not as ‘forgiving’ as a spinal fusion. The implants must be placed almost perfectly. This requires extra work and time, and sometimes these economics are not favorable to reimbursement.”
“I want to add that we still do fusions—both in the neck and low back—when it’s appropriate,” Blumenthal said. “We have found that in about 20% of the cases in the neck and 40% of those in the low back, fusion is the better option. Of course, these percentages favor disc replacement over fusion.”

Insurance Aspects of Artificial Disc Replacement
Dr. Guyer noted that while cervical disc replacement is being widely accepted and replacement in the lumbar area is slowly gaining acceptance, there are still challenges with insurance reimbursement for the life-changing technology. The procedure is not available to all patients.
“The cervical procedure has gained wide-spread acceptance,” Shellock said. “In fact, most carriers will cover cervical disc replacement. It is the lumbar procedure that has fallen behind a little.
“Interestingly, the lumbar has been around longer than the cervical. It’s not clear why some carriers are slow to come around, especially since we have had the outstanding results from the FDA testing. We still have a way to go. Many plans, including those that take care of our veterans and people who work for the government, are still being denied this type of procedure despite 23 years of data showing its benefits.”
When Is Fusion Called For?
“Years ago, with patients who were candidates for disc replacements, surgeons used the excuse that there were ‘too many disqualifiers’ to perform the procedure,” Guyer noted. “Just as with surgeons who perform hip replacement surgery, our philosophy has changed. If a patient has a bad hip, the surgeon will never recommend a hip fusion.
“Of the patients who are candidates for disc replacement, what are the percentages of those who should have a fusion?”
Dr. Shellock responded, “The vast majority of patients ARE candidates for disc replacement. My personal thought process is this: I’m trying to find a reason why a patient is NOT a candidate for disc replacement.”
“This is totally opposite from what the average spine surgeon does,” Guyer said. “Of course, we still do fusions, but because of our selection process, we get better results. For example, we just reviewed our first 1,800-disc replacement procedures, and our revision rate, where the implant is removed, was only 1.5% of the lumbar disc replacements. Total hip replacement, which is considered the ‘gold standard’ for replacement, has a 5% revision rate. Disc replacement is statistically more successful than hip replacement.”
Listen to this discussion here!
The Ideal Candidates for Disc Replacement
“With the cervical procedure, the patients who come into our office with a combination of neck pain and arm pain, may be a good candidate for disc replacement,” Dr. Shellock said. “In fact, most of the cases we see that are surgical treatments are candidates for disc replacement.
“These could be patients with spinal cord compression, spinal nerve compression, or degeneration of the disc. These are candidates that do great with disc replacement, and they can maintain motion.”
Dr. Blumenthal offers his thoughts on disc replacement in the lumbar spine area. “In the lower back area, the benefits would be to reduce or eliminate the pain and to preserve the motion. Artificial disc replacement is the only technology that can do both.
“The best candidates are the ones that have been told by another doctor that they need a fusion for his/her back pain. More than 50% will be candidates for motion preservation. Over the years, we have learned that decreasing the pain and maintaining the motion will decrease the need for future surgery when compared to fusion.”
The Future of Disc Replacement
“I believe there will be a marriage with navigation in the insertion of these devices,” Shellock predicted. “Our patients have enjoyed great success with this process, but I think we are moving toward robotics, navigation, and the reduction in the number of x-rays in the operating room.
“Technology is always advancing,” Blumenthal notes. “There will be advances in the materials for disc replacement. However, more importantly, it will come back to the surgeon. If you have one who knows when to do a fusion and when to do a disc replacement and has the experience to expand the group of potential patients, the procedure is more likely to be a success.
“So, if someone has been told they need a fusion procedure, I suggest they get another opinion from a disc replacement surgeon.”
Are you experiencing constant back pain? The spine experts at Texas Back Institute are world class. To arrange an appointment, just click here.