DAY 10 – Tuesday August 23rd:
Before heading to the Case operating room for surgery the team split up and saw post-surgical patients in the wards at Case and Mulago. At Mulago, Zbigniew, Siemionow and Jordan visited with three patients, who needed their surgical wound dressings to be changed. Patient J.S., a 35 year-old male was running a high fever since his surgery, while patient P.K. had trouble breathing at night, so required help from the BIPAP machine to breathe for him. Meanwhile in the clinic up the hill, Dr. Lieberman presented a lecture on congenital scoliosis to an audience of very interested surgeons and residents. It is important on our medical mission to make a lasting footprint by empowering the local physicians to improve their standard of care in addition to helping patients directly through surgery and consultation; we are only in Uganda for 2 weeks per year and must also think about the other 50. Even Master PT Professor Ngozi, PhD was asked to teach and present on key concepts in physical therapy – at both Case and Mulago.
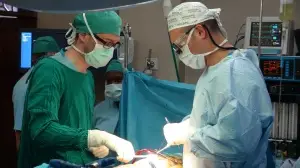
The surgical case today was a 15 year-old boy A.T. who suffered from persistent complications of tuberculosis. He had surgery in 2009 for post-TB complications, but afterward developed a chronic, draining infection. Now, his hardware had become loose and he had multiple levels of bony breakdown (osteolysis) and inadequate healing of bone (pseudarthrosis), with a substantial left-sided abscess. In May, he underwent a procedure to clean it out (debridement) but it was unsuccessful. Our plan was to repeat the debridement of the incision, abscess, and tract and to remove the loose broken hardware. During the surgery, it was impressive just how much granulomatous (gunky) tissue had been created by immune cells attacking the unresolved infection.
We saw three new patients today. The first was E.N., a 2 ½ year old girl with congenital scoliosis. Had we seen her last week, we might have been able to squeeze her in, but now due to time constraints she would have to wait until we return next year.
C.A. is a 24 year-old female with history of progressive leg weakness over three years and lower back pain. She had extreme lower extremity weakness (1/5 on the power scale) and allodynia, the sensation of pain in response to a non-painful stimulus (eg. gentle rubbing feels like burning). In the absence of imaging studies, Jordan and Dr. Ilalov exercised their differential diagnosis skills, ruling out vascular and autoimmune causes (the latter not at all common in Uganda) and suspecting a compressive lesion within her spinal cord, like a tumor. However, when Dr. Lieberman examined her he concurred that her symptoms are most consistent with a compressive lesion. It was then that she pulled out the secret X-rays of her back and it was clear that she had a focal kyphosis at the T11/12 disc level with a spondylolisthesis and disc resorption. Unfortunately, since the process had been going on for some time, the team felt that the damage was irreversible and surgery would be of minimal benefit. This was sad news to break, but having dealt with immobility for almost three years, it was not surprising to her.
The third patient was J.K., a 48 year-old male who was transferred from the trauma unit after a motor vehicle accident. Aside from being paralyzed from the shoulders down, he suffered a head injury and was confused and unable to speak (aphasic). He also had chemical burns over his body, but we could not illicit the history because of his head injury. His CT scan showed complete obliteration of the spinal canal (bone severed cervical spinal cord). This is the sad reality of spinal cord injury – and even in developed nations, motor vehicle accidents account for 50% of spinal injuries.
After a busy and interesting surgical challenge, Kirill didn’t have the stomach for dinner at the beautiful and sometimes delicious Serena hotel. Actually, he didn’t have the stomach for anything but a loading dose of Cipro. At dinner, the team howled at stories of spine missions passed (and present) and after the “Sister Sarah fiasco” yesterday, we did a “what time would Wednesday’s surgery begin” pool, Price is Right style: closest guess without going over wins!
Quote of the Day:
“Ugandance if you want to.” – Jordan & Dr. Ilalov (a team 362 effort)
Kirill examines a young woman at Mulago hospital. She has been losing mobility and strength in her legs over 3 years.
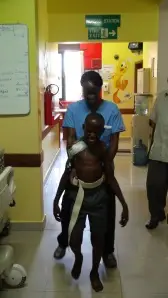
A post-operative young patient beams through the hard work of getting up and on his feet again.
It sure looks like Jordan’s getting the hang of this “doctoring” thing.
Dr. Siemionow examines a patient he has been working with and reports, “Everything is OK” in his cool, calm demeanor as always.