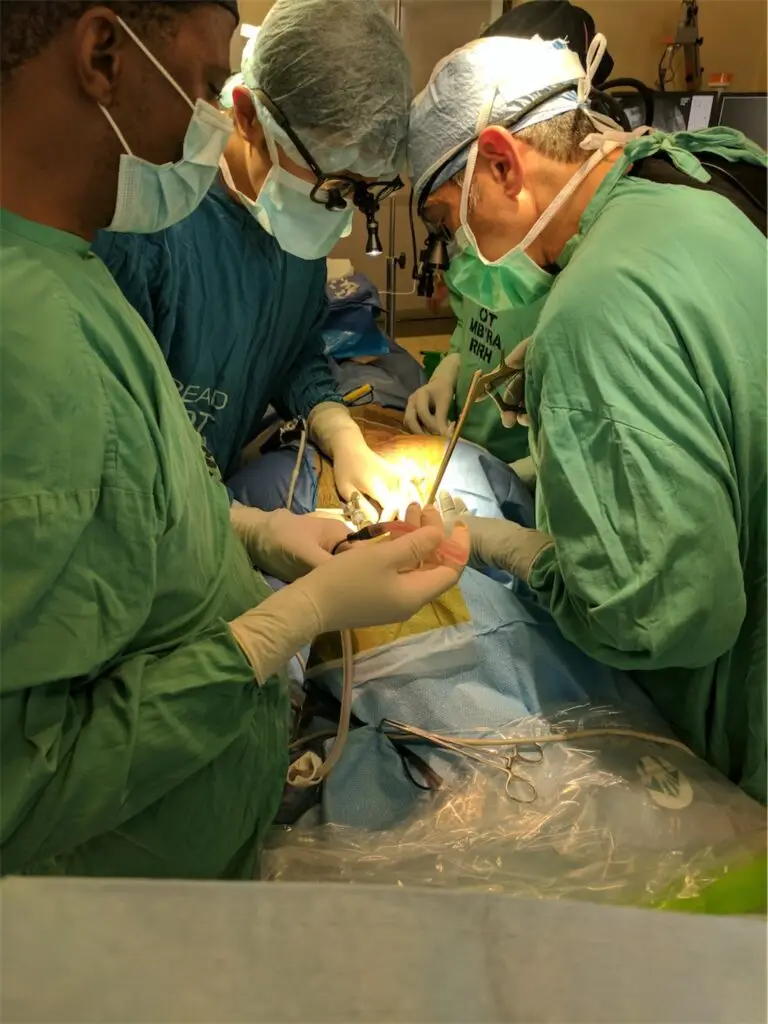
Day 5: Where’d that Patient Go?
As a premed student, there isn’t much I (Adam) can do in the operating room, but I’ve found other things to do. Taking notes on patients and keeping electronic copies of their records on a laptop, keeping track of possible surgical candidates, and probably the most important thing, keeping an up-to-date surgery schedule. Now, I’ve had no training and caught on fast on what to do, but Murphy’s Law caught me off guard, you know that line “Whatever can go wrong, will go wrong”? I made the mistake of almost forgetting it.
The day was going to be a good length; not long, not short. Four cases were planned; the removal and biopsy of a mass on a girl named Rebecca, an ACDF (Anterior Cervical Diseconomy and Fusion; it’s done remove bad disc [padding between vertebrae] and fuse the bones together) on a woman named Jolly, a decompression on a gentleman named George, and a simple injection to attempt to alleviate pain on another man by the name of Nehemiah.
Dr. Huang and I went on rounds again, visiting patients from all the days prior we had operated on. Wednesday’s patients, Bernard, Norah, and Medias K, were all feeling some post-op pain (to be expected), but doing alright. Derick, with his prior condition, could not communicate to us, but his parents stated that they saw improvement already. The patients from days prior, Denis, Medias, and now Godson, were all beginning to do even better; some saw larger improvements than others, but none the less, all were improving. Julius, however, was beginning to complain of a new pain in his hip, but his strength was okay. It was at the end of the rounds, we noticed a patient we had seen prior to the clinic, a boy with head trauma and inability to move his head side to side or forward, had returned, with the MRI we had requested to check for spinal cord damage. We spoke briefly to the boy, Antony, took the MRI and planned to look at it with Dr. Perry.
As usual at this point, we headed back to the OR, where we went our separate ways; he went to join those performing surgery, while I checked on both operating rooms, and inform Dr. Perry that the boy’s MRI was in my possession. Not long after I told her, she finished her decompression, and looked at the MRI, noting nothing unusual; the spinal cord looked perfect, and gave me directions to tell him; he could come out from the collar he was in, take muscle relaxants, do physical therapy, and no contact sports for 3 to 6 months because of a concussion as well.
I searched for Natasha, and together we went to inform Antony and his mother, as well as ask physical therapy to start working with him. They came, and feeling uncertain about working with him, asked us to take him to their neurologist, who then cleared him, saying there was no damage he could see either, but he should hold on the physical. We spoke with the family a little more and discharged them.
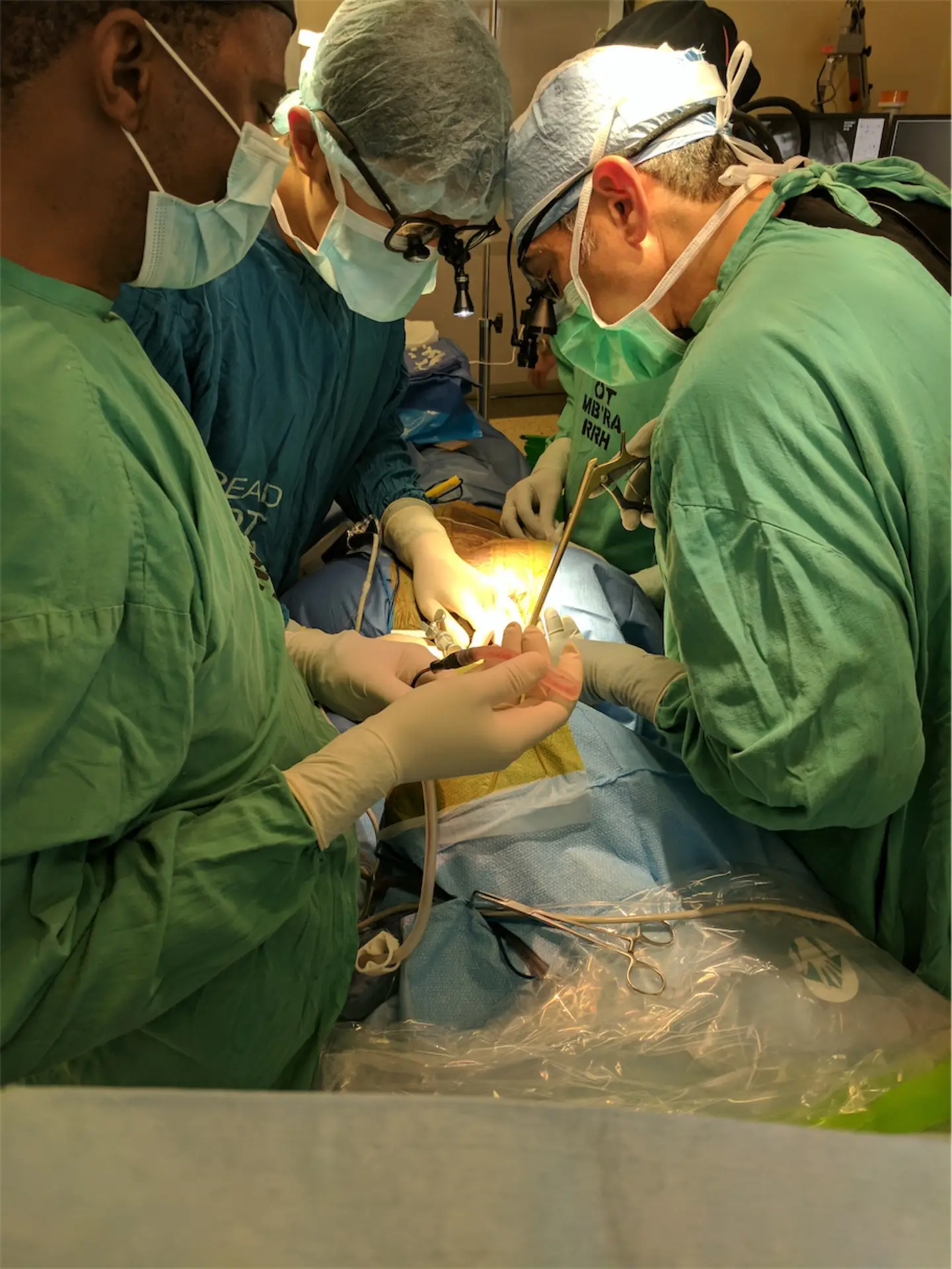
Natasha, who’s in charge of the surgical ward and prepping patients for surgery, and I made our way back to the OR when she informed me that prior to this, she was having difficulty finding Rebecca for her surgery. I was confident we’d locate her, no problem. I headed into the OR with Dr. Lieberman, thinking he’d be only halfway done, only to discover that, no, he was close to done. Oh boy. I checked on them and quickly left to find Dr. Stanly Kisinde, a local doctor who was very close to the team, to see if he if had any idea where the girl was only to discover that he, too, was searching for her. He told me to wait before I told Dr. Lieberman, and quickly called the contact info we had, only to discover she wasn’t here.
Okay, okay. Now to tell Lieberman.
I head into the room I know Lieberman is in, only to see him walking out. I inform him that she wasn’t present. After a short discussion between doctors, it was determined that we’d simply move up the 4th case for the day, the epidural injection. In addition to this whole fiasco, Sherri, who was scrubbed at the time began experiencing some stomach distress. Dr. Perry quickly came to the rescue and assumed the role of scrub tech until the case was completed.
With everything under control, I went to watch the injection, but had to leave early to assist in prepping the surgery list for the following day. Natasha and I spoke again, giving each other information, and getting the status on the x-rays. She calmly informed me that one patient is unable to get their x-ray, as they can’t walk. We discussed possible ideas and parted ways. I met up with the rest of the crew at the end of an early day, and waited for Brian, who wasn’t feeling very good, (we believe he caught a cold from the draft wafting through his torn disposable scrubs). We went to finish prepping the tools for the following day. Once wrapped up, and patients tucked in, we went out to an early dinner. We again shared our lessons of the day, from which Brian and Sherrie (who was feeling better at this point) provided the back to back, quotes of the day, which caused us all to burst into laughter.
Our quotes for the day:
“There are no sick days in spine.” Brian Failla
“You’ve gotta know when to tap out.” Sherri LaCivita
With an early dinner in our stomachs and returning to the hotel, we decided to once again play Jenga, as Dr. Perry had never played Jenga. Work hard, play hard, you know? And let me tell you, playing that game with three surgeons is the most intense way to play it. We split into teams, Girls (Sherri, Kari, and Dr. Perry) VS Boys (Dr. Lieberman, Dr. Huang, and I), and thanks to Kari “Oops” Zagar, hitting the table with her knee in the All-Or-Nothing game, boys took it 3/0. Thanks Kari!
It was after this, knowing we had a long day on Friday, that we decided to call it a night and get our rest. We knew we’d need it.